Archives
Obesity Strongly Associated with COPD In “Never-Smokers”
 Chronic Obstructive Pulmonary Disease (COPD) is much more common among never-smoking older women who are morbidly obese (having a body mass index of 40 or higher) than among their female peers in the normal weight range. Morbidly obese older men who have never smoked also had a much higher prevalence of COPD than never-smoking men who were normal weight, reported lead author professor Esme Fuller-Thomson, Sandra Rotman, endowed chair at University of Toronto's Factor-Inwentash Faculty of Social Work and Department of Family and Community and director of the Institute for Life Course and Aging.
Chronic Obstructive Pulmonary Disease (COPD) is much more common among never-smoking older women who are morbidly obese (having a body mass index of 40 or higher) than among their female peers in the normal weight range. Morbidly obese older men who have never smoked also had a much higher prevalence of COPD than never-smoking men who were normal weight, reported lead author professor Esme Fuller-Thomson, Sandra Rotman, endowed chair at University of Toronto's Factor-Inwentash Faculty of Social Work and Department of Family and Community and director of the Institute for Life Course and Aging.
“Surprisingly few studies have focused on never-smoking COPD patients,” said co-author Senyo Agbeyaka, a graduate of the University of Toronto's Factor-Inwentash Faculty of Social Work. “We wanted to address this gap in the literature by examining which factors are associated with COPD among never smokers aged 50 and older.”
COPD is the third leading cause of death in the U.S.
In addition to obesity, older age and lower income were associated with COPD among both men and women. Among women, but not men, height and education level were negatively associated with COPD, but being married was associated with higher odds of COPD, the report found.
The study was based on a nationally representative sample of non-Hispanic white respondents aged 50 and older who reported that they had never smoked. Data were drawn from the 2012 Center for Disease Control's Behavioral Risk Factor Surveillance System. The final sample included more than 110,000 respondents, of whom almost 4,000 were morbidly obese and 5,000 reported that they had been diagnosed with COPD.
The survey did not allow researchers to identify why older obese Americans who were never smokers had such a high prevalence of COPD. "These findings highlight the importance of health care professionals routinely screening their older obese patients for COPD, even when the patients have no history of smoking" said professor Esme Fuller-Thomson.
COPD is a group of progressive lung disorders that make breathing difficult, including emphysema and chronic bronchitis. The best-known risk factor for COPD is smoking, but one-quarter of COPD patients have never smoked.
E-Cigarettes: Teens 'Should Not be Using Them at All'
 Often used as an alternative to traditional cigarettes, e-cigarettes are battery-powered devices that frequently contain nicotine solutions. Although many adults use these devices for smoking cessation purposes, “researchers have raised concerns that teenagers may be using them as a gateway into this very habit.” Use of e-cigarettes is prevalent among teenagers, despite the fact that they are banned for sale to individuals under the age of 18.
Often used as an alternative to traditional cigarettes, e-cigarettes are battery-powered devices that frequently contain nicotine solutions. Although many adults use these devices for smoking cessation purposes, “researchers have raised concerns that teenagers may be using them as a gateway into this very habit.” Use of e-cigarettes is prevalent among teenagers, despite the fact that they are banned for sale to individuals under the age of 18.
A recent research study published in Pediatrics, the official journal of the American Academy of Pediatrics, has revealed far more serious outcomes associated with use of e-cigarettes than nicotine addiction and the possible transition to cigarettes.
Dr. Mark L. Rubinstein, the lead study author, and his team at the University of California, San Francisco discovered that teenagers known to "vape" could in fact “be exposing themselves to dangerous chemicals that have been linked to cancer.” It is critical that teenagers are informed that toxic substances are contained in both e-cigarettes and in traditional ones, and even nicotine-free devices may still be harmful.
“Teenagers need to be warned that the vapor produced by e-cigarettes is not harmless water vapor, but actually contains some of the same toxic chemicals found in smoke from traditional cigarettes. Teenagers should be inhaling air, not products with toxins in them,” said Dr. Rubinstein.
The researchers collected and analyzed 104 adolescents’ urine samples, 67 of who used e-cigarettes and 17 of who used both e-cigarettes and traditional cigarettes. The other twenty teenagers neither smoked nor vaped. Based on their study, Dr. Rubinstein and his team determined that teenagers who used e-cigarettes “had a three times higher concentration of toxic compounds in their bodies than their non-vaping peers.”
Rubinstein’s study was the first of its kind to test for harmful carcinogenic substances including chemicals such as “acrylonitrile, acrolein, propylene oxide, acrylamide, and crotonaldehyde,” among teenagers who use e-cigarettes. Each one of these toxins have been labeled as either carcinogenic or potentially carcinogenic to humans.
Researchers also discovered that some of the substances that were discovered in the bodies of adolescents using “flavored, nicotine-free e-cigarette liquid,” such as propylene glycol and glycerol, have been shown to create carcinogenic compounds if they are heated.
"When they're heated to the high temperatures required for vaporization, they can produce toxic substances that are potentially carcinogenic," said Dr. Rubinstein.
Trial of New Triple Inhaler Shows 20 Percent Reduction in COPD Flare-Ups
A recent study published in Lancet, suggests that flare-ups resulting from chronic obstructive pulmonary disease (COPD) can be reduced by 20 percent through the use of a combined triple inhaler.
Researchers from The University of Manchester conducted a year-long trial involving 2,691 patients who were current or former smokers with COPD. Over a thousand participants were provided with a new inhaler that contained three different compounds, another thousand were provided with the most commonly used inhaler, and 500 were provided with two inhalers that contained the triple combination.
 On average, patients experience 1.3 exacerbations per year. These commonly result from infections that can lead to hospitalizations, faster progressions of the condition and even death. Yet, researchers discovered that, “the risk of an exacerbation was reduced by 20 percent in the group using the triple inhaler.”
On average, patients experience 1.3 exacerbations per year. These commonly result from infections that can lead to hospitalizations, faster progressions of the condition and even death. Yet, researchers discovered that, “the risk of an exacerbation was reduced by 20 percent in the group using the triple inhaler.”
"This is the first long-term study to look at the possibilities of triple therapy as a preventative measure for COPD exacerbations,” said Jørgen Vestbo, Professor of Respiratory Medicine at The University of Manchester. "COPD exacerbations lead to approximately 150,000 hospital admissions and 1.2 million bed-days every year in the UK, so to reduce this figure by 20 percent would make a huge difference, not only for patients' quality of life, but also for the resources of the NHS."
Researchers also discovered that the triple combination inhaler also aided in improving lung function and helped to reduce overall symptoms. Additionally, the study is the first of its kind to, “study a biomarker for individualizing treatment.” Through the use of a blood eosinophil, researchers were able to identify patients, “more likely to have even greater benefit from the triple inhaler containing an inhaled steroid.”
Could New FDA E-Cigarette Regulations Help More People Quit Smoking?
 At the current juncture, electronic cigarettes, or e-cigs, are not nationally regulated as a tobacco and help contribute to lung diseases such as emphysema and chronic obstructive pulmonary disease (COPD), the third leading cause of death nationwide. Additionally, smoking is the leading preventable cause of death in the world. So, if the problem is so large, why have e-cigarettes not yet been regulated nation-wide?
At the current juncture, electronic cigarettes, or e-cigs, are not nationally regulated as a tobacco and help contribute to lung diseases such as emphysema and chronic obstructive pulmonary disease (COPD), the third leading cause of death nationwide. Additionally, smoking is the leading preventable cause of death in the world. So, if the problem is so large, why have e-cigarettes not yet been regulated nation-wide?
The Food and Drug Administration (FDA) has recently proposed polices that would include e-cigs as tobacco products and specifically include them in the Family Smoking Prevention and Tobacco Control Act that was signed into law by President Obama. The FDA is still aiming to extend other tobacco laws to include e-cigs, since the FDA oversight was limited to solely include cigarettes.
Because the decision to create nationwide regulations has already taken nearly a year to rule on, some “state and local jurisdictions have stepped in to pass laws and policies within their authority.” These policies include minimum age of purchase laws, location limitations of where e-cigs can be used (much like those of traditional cigarettes), and the additional taxes for the purchase of e-cigs and the associated accessories.
While these policies can be useful as a temporary fix, state laws can change often and quickly so the FDA will need to move quickly in order to create “rules and regulations that will achieve the greatest population health benefit and result in the beginning of the end of smoking as we know it.”
Click Here to Access the Full Story on U.S. News and World Report
COPD, Asthma Now Can Be Studied Outside the Body
 Have you ever heard of organ-on-a-chip? If you haven’t, you may soon. Researchers at Wyss Institute for Biologically Inspired Engineering at Harvard University recently developed a model of the human small airway to help study lung inflammatory diseases, such as asthma and chronic obstructive pulmonary disease (COPD), outside of the body.
Have you ever heard of organ-on-a-chip? If you haven’t, you may soon. Researchers at Wyss Institute for Biologically Inspired Engineering at Harvard University recently developed a model of the human small airway to help study lung inflammatory diseases, such as asthma and chronic obstructive pulmonary disease (COPD), outside of the body.
This development will help to “gain new insights into the disease mechanisms, identify novel biomarkers, and test new drug candidates”, without the invasiveness and costs associated with surgery. Additionally, the researchers also created a “microfluidic model of the lung small airway that recapitulates critical features of asthma and COPD”, which gives the team “a window on molecular-scale activities in the context of living human lung tissue.”
The team also noted that the organ-on-a-chip can be utilized as a discovery platform for disease-specific drugs and biomarkers. This means that “drugs targeting different key molecular components of inflammatory pathways can potently suppress pathological processes in asthma and COPD-tailored small airway chips.”
The organ-on-a-chip technology is helping to not only map out how COPD affects the human body, but how personalized treatments can be identified and created to help improve quality of life.
Assessment of the Patient — Your Evaluation as a Possible COPD Patient
Here is a personal checklist that will enable you to determine whether you should consult your physician.
-
Does COPD run in my family?
-
Do I smoke?
-
Am I short of breath more than others?
-
Do I cough?
-
When I cough, do I cough up yellow or green mucus?
History
A careful history, with a focus on cough, expectoration, shortness of breath, wheeze, and the duration of these symptoms is basic. A careful smoking history and an occupational history detailing possible dust and/or irritant exposures are also needed. Most patients have had some telltale symptoms for years before they come to a doctor for an evaluation. None of these symptoms is specific or diagnostic by itself. A careful family history in reference to close relatives with COPD is important because COPD runs in families. Some common questions often asked by doctors or nurses to help evaluate the patient are listed in Tables 1 and 2. It is important to talk about the patient’s duration of symptoms, lifestyle, work environment, and problems related to the illness.
Physical examination
A complete physical examination should be performed during your first visit to a doctor.
Table 1: Questions a doctor may ask:
-
How long have you had cough, shortness of breath, or wheeze?
-
Have you seen many doctors for it? What are you now doing to treat it?
-
How many days did you miss from work last year because of the lung problem?
-
Were you in the hospital for it? How long and how many times last year?
-
Describe your usual good day.
-
Do you have more good days than bad days in a week? What are you able to do when you are feeling your very best?
-
Who do you live with?
-
What recreation do you prefer?
Table 2: More Questions Your Doctor or Nurse May Ask:
-
How does the emphysema or chronic bronchitis bother you?
-
When does it bother you the most?
-
What have you learned to do that helps you to live with it?
-
Does it ever embarrass you to have lung trouble?
Your physician will thoroughly examine your chest, observe your breathing patterns, and perhaps monitor how hard you are working to breathe. He or she will note the degree of over-inflation by percussion (tapping over the lungs). He will listen to your chest with a stethoscope to hear the air flow in and out of your lungs. The intensity (loudness) of the sounds is helpful. Noises caused by mucus or inflammation are also noted.
The physician or nurse will also listen to your heart sounds to determine the rate and rhythm of your heart and any signs of heart strain that may accompany advanced stages of COPD. The examination itself is not very accurate in determining the severity of the abnormality, however. A physical examination may be normal even in the early stages of significant disease. This is because airflow abnormalities are usually moderately advanced before they can be detected with a stethoscope!
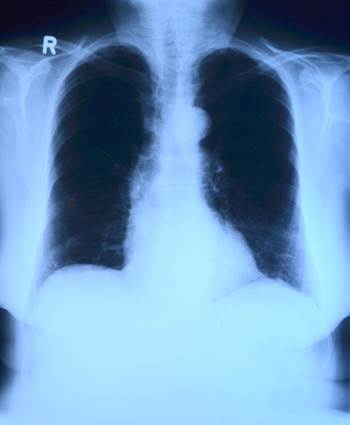
Chest X-ray
Chest x-rays are not very useful in assessing the patient with COPD. By the time the x-ray is clearly indicative of the disease, the neighbors usually know the diagnosis! However, the x-ray may show over-inflation of the lungs, which is common in emphysema. X-rays are also valuable in finding other abnormalities such as shadows which may indicate coexisting lung cancer. Lung cancer and COPD often occur together because both are caused by smoking. The heart and the large vessels to and from the heart can also be seen on a chest x-ray and give some indication about associated heart strain, but only in advanced stages of disease. However, the chest x-ray can be completely normal, even when the patient has a significant degree of COPD. The x-ray, though traditional, is not a good way of diagnosing or evaluating COPD.
Electrocardiogram (EKG)
The EKG also is not useful in evaluating patients with COPD. In very advanced disease, EKG abnormalities are usually evidence of strain in the right side of the heart, i.e., that portion of the pump that propels blood from the tissue back through the lungs to take on oxygen and get rid of carbon dioxide.
Sputum Examination
Culturing the sputum of patients with emphysema and/or chronic bronchitis is almost useless. The common bacteria are well-known, and today physicians properly prescribe antibiotics based on their knowledge of the most common organisms and will do so if sputum increases in volume and becomes colored. Yellow or greenish sputum is almost always infected and requires antibiotics.
Measuring Lung Capacity
A simple device called a spirometer measures your lung capacity. During this test you take a deep breath, as deeply as you can, and blow it out all at once into a machine that records airflow and capacity. The total amount of air blown out of fully inflated lungs is called the vital capacity. Since the air is forced out by your muscular effort, it is called forced vital capacity (FVC, newer term FEV6). This test measures the useful size of your lungs. The rate of airflow tells how open the air passages are and how well the lungs can empty, or how well their elasticity is functioning. The lungs empty somewhat like an inflated balloon. Remember how a flabby or overused balloon empties slowly and incompletely? This is a lot like the lung with emphysema. The airflow test is called the forced expiratory volume in one second, since this airflow is timed or measured over the first second of exhalation. The symbol for forced expiratory volume in one second is FEV1. These two tests, the FVC and FEV1, reveal all your doctor needs to know about your lung capacity and airflow. These two numbers are somewhat similar to systolic and diastolic numbers in blood pressure readings. We believe that knowledge of FVC and FEV1 is as valuable and important to health promotion as knowledge of blood pressure. These tests measure your lung power, which is essential to your continuation and enjoyment of life.
Normal values are based on age, sex, and height. Younger and taller individuals have greater airflow and air volume than shorter or older people. Men have slightly greater airflow and air volume compared with women of the same age and height.
Self-Testing- Try It Yourself
Normal lungs have large volume, and they empty quickly because airways are open and lungs are elastic. You can do a little checking yourself with a stopwatch. Take a full breath; hold if for one second. Then, with your mouth open, blow out as hard and fast as you can. Your lungs should be completely emptied – meaning that you can blow no more air out even though you try– in no more than 4 to 6 seconds.
If one takes longer to blow out all the air, it means that airflow is obstructed or limited. Today we use the term “limited” because this airflow reduction can be due to either a loss of lung elasticity (emphysema) or problems with airways (asthmatic or chronic bronchitis). See how simple it is!
Unfortunately, routine lung function tests have been accepted all too slowly. No person would go for a complete check-up if the physician did not examine the eyes, ears, nose, throat, listen to the heart and lungs, feel the abdomen for any abnormal masses, and examine the genital, rectal, and pelvic areas. All these are routine, and to supplement them, appropriate laboratory blood and urine tests are done, plus an electrocardiogram and, usually, a chest x-ray. Unfortunately, none of these examinations or tests identifies early COPD.
Only spirometric measurements of the kind we have just described can identify the patient who is just beginning to develop a lung abnormality.
When one considers that the disease process finally resulting in disability may go on for 20 to 30 years, doesn’t it make sense to identify the problem early and to take immediate corrective action? The answer must be yes if you are to a enjoy a long happy life.
Very simple devices for measuring lung capacity are becoming popular. One such device is called a peak flow meter, which measures the greatest airflow rate you can produce. A man’s normal figure is around 600 liters per minute, and a woman’s is 370 liters per minute. Both are normal. (The lower value for women is because of their shorter stature and female sex). Some physicians instruct their patients to use peak flow meters at home to study the response to treatments designed to open up their air passages. Another new device called a spirometer accurately measures forced vital capacity. These measurements of both volume capacity (forced vital capacity) and flow can give a good estimate of the mechanical function of the lungs. (Newer, less expensive pulmonary function testing equipment is now readily available for use in primary care physician offices).
Other tests are used in more advanced stages of disease to obtain additional knowledge about the lungs’ function. One such test is the blood gas measurement. A small amount of blood is drawn from an artery by a small needle and syringe. This blood is analyzed to measure the amount of oxygen and carbon dioxide it contains. This test is used to assess more advanced stages of emphysema and chronic bronchitis and is needed when the physician is considering prescribing oxygen and in cases of serious and emergency illness.
Another simple method of measuring blood oxygen is with an instrument called an oximeter which is widely used today. It is popular because it does not require arterial blood sampling. However, it is not as accurate as arterial blood measurement, and it tells nothing about the levels of carbon dioxide or acid (pH) in the blood. The pulse oximeter measures blood oxygen by reflected light. This test is easy and painless and will be much more widely used in the future.
Additional lung function tests such as the diffusion test also measure the integrity of the air-blood interface, or alveolar capillary membrane. Numerous additional tests are used for research purposes, but they do not have any practical value at the present time.
In summary, adequate evaluation of patients with all stages of COPD is within the reach of all doctors and their patients. The approach is simple and straightforward. All patients with shortness of breath, cough, wheeze – particularly those with family history of COPD and absolutely all smokers – should insist on this crucial evaluation.

Answers from Dr. Thomas Petty, Professor of Medicine, University of Colorado.
Is Prednisone a Friend or Foe?
Probably just about everyone who reads this monthly Newsletter knows about prednisone. Prednisone is in a class of drugs called corticosteroids, related to the cortisone group of medications. These drugs are highly useful in the management of asthma and some patients with COPD, and, quite frankly, I couldn’t get along without them in my practice. This statement has to be tempered with the clear understanding of what I call the “downside” of these valuable drugs, and these can be substantial. Yet many of the side effects can be avoided or minimized with certain strategies.
Prednisone is an anti-inflammatory drug and thus deals with inflammation of the conducting air passages in the lung. Inflammation may be present in both asthma and COPD. The strategic use of prednisone can soothe and thus heal the delicate lining layer of these passageways, making them more resistant to bronchospasm. Prednisone has another effect in preserving or even increasing the receptors for inhaled bronchodilators. Thus prednisone is used both to combat inflammation and to enhance the effectiveness of one of the most valuable bronchodilators we have for asthma and COPD. The downside is well-known. It causes wear and tear on the bones, and in some patients the acceleration of cataract formation and the worsening of glaucoma (high pressure in the eyes). The bone problem is much worse in women than men, and it is a particular problem in small-boned, light-skinned women beyond the menopause. On the other hand, large-boned, dark-skinned people have relatively little trouble with prednisone. Men have far less trouble than women, probably because their bones are larger to start with. The bone problem (osteoporosis) can be largely prevented by the appropriate use of calcium. A quart of skim milk gives 1,000 mg of calcium, and simple medications such as Tums contain a lot of calcium. Physicians believe that between 1,000-1,500 mg per day is necessary to help prevent osteoporosis. Exercise also helps protect the bones, and, of course, being able to breathe makes this exercise possible. (Newer medications have become available to help treat osteoporosis).
Anybody receiving long-term prednisone should have an annual eye exam and, of course, plenty of people have cataracts and glaucoma without the use of steroids. If steroids are making things worse, that fact can be dealt with by using medications and surgery. Short courses of prednisone cause almost no harm, and even low maintenance doses given each morning or evening in a single daily dose have minimal side effects in most patients. Most of the other rumors about prednisone are blown way out of proportion, but it is true that some folks have more trouble from prednisone than others. It’s hard to discuss all of the ins and outs of prednisone therapy in one short Newsletter, but the “bottom line” is prednisone is very useful in many patients and usually does a lot more good than harm. I’ll be in touch with you next month with more information on prednisone and some additional tips which may be interest.
(NOTE: Prednisone can also have an effect on blood sugar levels, which may be of importance to diabetics).

Dr. Thomas Petty, Professor of Medicine University of Colorado Health Sciences Center; Consultant and Faculty at HealthONE Center Denver, CO.
It’s Never Too Late to Stop Smoking
Almost everyone knows of the harmful effects of tobacco smoke. It has been conservatively estimated that regular smokers of cigarettes sacrifice seven years of life. If one divides the number of cigarettes smoked in a lifetime on the average into this seven years loss, it turns out to be 5 ½ minutes for each cigarette! What an astonishing statistic. The premature loss of life is primarily due to doubling the risk of heart attack, lung cancer, and emphysema. There are other cancers such as bladder, larynx, esophagus, pancreas, and uterus which are also caused by tobacco. Thus, it becomes pretty clear that stopping smoking is critical to future health. Never starting, of course, is better.
"But I have already smoked too long, doctor" is a common statement of my patients. “It won’t do me any good now because too much damage is already done,” they will continue. Nothing could be further from the truth. It is now known that there is benefit from stopping smoking no matter how long you have smoked. The risk of heart attack returns to normal after five years of non-smoking, and cancer risk goes way down also after five years or more of smoking cessation. In emphysema, the rate of loss of breathing capacity slows once people finally stop. Even patients over the age of 60 with advanced degrees of impairment live longer if they stop smoking. Thus, it is pretty obvious that no one should continue to smoke no matter what their preconceived notions about damage already done may be.
But how to stop—-ah-h-h—that’s the question! There is no simple answer. A personal commitment to quitting is, of course, fundamental. Setting a date for stopping, substitution with candies, chewing gum or something else to chew on helps a bit. Nicotine containing gum is useful in many patients in dealing with the withdrawal symptoms which plague many nicotine addicts. Nicotine patches and nasal spray are also effective. The changing of life patterns and avoiding social signals which call for a cigarette is also extremely helpful. There is no way that I can tell everyone who reads this newsletter exactly how to stop smoking, but in fact, nearly everyone can stop now. It is not really later than you think. Plan for your first no smoking day in a long time soon because, after all, "it is the first day of the rest of your life."

Thomas L. Petty, M.D., Professor of Medicine, University of Colorado.
Will They Ever Find a Cure for Asthma?
As a clinician and clinical scientist, and one who likes to speak to public groups, I am often asked the question, which is the title of this month’s newsletter. Yes, friends, there will be cures to most diseases, but let’s limit the discussion to the common problem of pulmonary disease.
Asthma is a problem for both the young and old, and it can be mild or severe. Air passages are obstructed with asthma both intermittently and chronically. New developments and understanding of basic asthma mechanism are being reported almost daily. The discovery of these mechanisms leads to new drugs and treatment strategies, which are equally important. Today, we recognize asthma as having two major factors, i.e., a bronchospastic factor when there is a sudden muscular narrowing of air passages, and an inflammatory factor which also narrows the air passages and creates mucus. A growing number of potent bronchodilators can open up air passages by relaxing these airway muscles. Today, there is more focus on methods of preventing or treating inflammation. In more pure forms of asthma, a drug Cromolyn (Intal) is an excellent preventative for many people. It is useful in both children and adults. It doesn’t do anything for established inflammation, however. Active inflammation requires our old “friends,” the corticosteroids, namely prednisone. In other newsletters, I have pointed out that prednisone is much more of a friend than a foe. It can be used strategically to combat active inflammation. Some individuals also require prednisone on a regular basis to prevent the progress of the disease. Inhaled corticosteroids, i.e., beclomethasone, bedenoside, flunisolide, fluticasone, triamcinolone, may also be effective in some patients with COPD, but mostly these are patients who primarily suffer from asthma. Additional drugs that are not related to the cortisone family are under study, and I am sure that within a number of years we will have alternate approaches to the problem of inflammation in bronchial asthma.
COPD is more persistent and progressive form of airflow obstruction and includes Asthmatic Bronchitis, Chronic Bronchitis, and Emphysema. Stopping smoking is the answer to prevention and progression of COPD. By stopping all smoking, the great majority of patients could avoid COPD altogether or could stop it in its tracks. Those patients with the rare form of congenital alpha 1 antitrypsin deficiency can now have a replacement therapy. The alpha antiproteinase is called prolastin. It requires weekly or possibly only monthly infusions. In effect, it is a cure because it replaces the basic deficiency. But, it is not for all forms of COPD. (Two other forms of treatment for alpha 1 deficiency have just been introduced).
Lung cancer is now the most common malignancy in both men and women. Smoking causes approximately 85% of lung cancer. Thus, we already have a cure for 100,000 men and 50,000 women who will get lung cancer each year! Stopping smoking is the answer to prevention. Otherwise, the cure for lung cancer is surgery, if it is possible. Chemotherapy and radiation are not very effective, but new lung cancer centers are being developed. These will focus upon early identification and intervention, and, of course, this will also mean smoking cessation. Hopefully, the newer drugs for lung cancer will be found more effective.
What about acute respiratory insults? The major lung disease spectrum cited here is the adult respiratory distress syndrome first described by the Denver group. This affects 150,000 patients each year. We are proud of the fact that 40-50% of ARDS patients survive, through therapies designed in Denver and now applied worldwide. We are also searching for better methods of prevention, and new drugs can help prevent acute lung injuries.

Dr. Thomas Petty, Professor of Medicine University of Colorado Health Sciences Center; Consultant and Faculty at HealthONE Center Denver, CO.
When You Can’t Sleep
Insomnia, that is, the inability to fall asleep and stay asleep at appropriate times is a very common problem. I venture to say that nearly every person has had some degree of sleeplessness at one time or another. I am not talking about the restlessness of anticipation, such as just before holidays, big trips, or other special events. I am talking about when there is nothing particularly on your mind, either good or bad, and you just can’t sleep.
The basic reasons underlying sleeplessness are the subject of a great amount of study these days. Sometimes there is a clear-cut explanation, such as lack of oxygen during sleep or so-called sleep disordered breathing. Your see that our respiratory center has a lot to do with rate and depth of breathing during sleep, and if your respiratory center is getting mixed messages about how to breathe in case of emphysema, breathing regularity may become disturbed or temporarily interrupted. This will almost always awaken a patient because of the sensation that “something is wrong.”
When these definite abnormalities are found by a physician, specific corrective treatment can be prescribed. Many more patients have sleep disturbances for no known reason. Here is some advice about dealing with this common situation.
First, just recognize that sleeplessness is common and, by itself, is not harmful. Just remember that you will sleep the next day. If things are running through your mind or you are afraid of forgetting something important, turn on the light and make notes of your ideas, thoughts, or concerns. This will break the cycle of “things running through your mind.” It is even good to get up and do natural things that will promote sleepiness, such as reading, taking a warm bath, or drinking some warm milk. Why do these things work? Simply stated, they relax your mind so that natural sleep occurs, and there is a substance in warm milk called tryptophan which makes people sleepy.
I have left sleeping pills to last because they tend to be overused, but in certain situations mild amounts of tranquilizers or short-acting sleeping pills can be prescribed with safety by your doctor. Before relying on sleeping pills, just remember that some degree of insomnia is very common. In fact, that is why I am writing this Newsletter at 2:00 in the morning.

Dr. Thomas Petty, Professor of Medicine University of Colorado Health Sciences Center; Consultant and Faculty at HealthONE Center Denver, CO.




